Avalere Analysis: Exchange Consumer Experience
Summary
Study finds lack of transparency on drug coverage in exchanges, but better data on provider networks.A new Avalere Health analysis of the consumer shopping experience in health insurance exchanges reveals that provider network directories are very or moderately accessible to consumers in 76 percent of plans analyzed, but drug formularies are very or moderately accessible in only 52 percent of plans. Thirty-eight percent of plans had no drug formulary data available, presenting significant obstacles to consumers who are shopping for insurance and attempting to assess the value of their coverage.
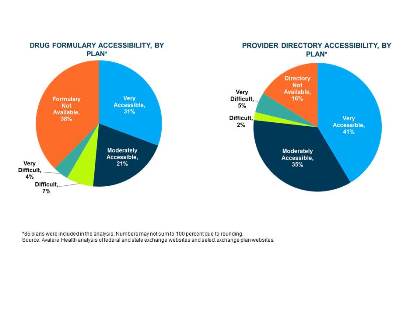
For the analysis, Avalere analyzed formulary and provider directory accessibility among plans sold in five states via HealthCare.gov and through 12 state-based exchange websites. HealthCare.gov and several other state websites-including Colorado, Connecticut, Maryland, Minnesota, Nevada and New York-include a link to formularies and provider directories for each plan. However, the links are not always direct, and in some cases, these links may redirect consumers to the insurer’s homepage, which requires consumers to navigate the website (with as many as six clicks) to find the appropriate documents.
“As the open enrollment period for the inaugural year of the exchanges has just ended, it is a good time to take stock of the consumer shopping experience and identify ways to improve transparency in future years,” said Caroline Pearson, vice president at Avalere Heath. “Providing understandable and accessible information about the providers and drugs included in exchange plans is essential to helping enrollees make informed purchasing decisions that balance premium against scope of coverage.”
In 2014, exchange websites present a variety of options for sorting plan options. Most exchanges by default list plans by premium price (low to high), but some websites offer the functionality of sorting by other features (e.g., metal level, carrier, benefit design features). California has the only website that offers consumers a rough out-of-pocket calculator to help gauge expected costs by exchange plan. Nevada is the only website that includes a drug search function that shows how a person’s drug is covered by every plan on the exchange.
Methodology:
Avalere analyzed the exchange websites that enable consumers to shop and compare individual insurance plans. Avalere reviewed plans sold in the Federally-Facilitated Marketplace (FFM) on HealthCare.gov and the other state-based exchanges (SBEs). For each website, Avalere analyzed five plans: the two lowest-priced Bronze and Silver plans and the lowest-priced Gold plan (five plans per state). For the FFM website, we analyzed five plans in the top five states by projected enrollment. Avalere selected the most populous counties in each state for the analysis. Avalere could not access exchange websites for Hawaii, Kentucky, or Vermont.
We gauged the consumer experience on several factors, including the ease of accessing formularies and provider directories, the order of plans listed on websites, and the availability of out-of-pocket calculators and drug look up tools. Avalere assessed access to formularies and provider directories by devising a scoring methodology specific to this information. To determine a score for each analyzed plan, Avalere assigned a score based on the following: (1) number of clicks to access the information; and (2) location of the information (assigned a score based on Table 1). As a note, Avalere started the counting of clicks at the point of viewing the list of plan options for a given exchange website. From there, we summed the two numbers to get a total score for each plan. The scores fall into five broad categories of accessibility (outlined in Table 2). For example, a formulary directly linked from an exchange website that took 2 clicks to access would receive a score of Very Accessible (0 for exchange location plus 2 for the clicks).
This analysis was funded by Pfizer, Inc. Avalere maintained editorial control over the content of the analysis and release.
View Avalere’s full exchange consumer analysis attached.
For more information about exchange consumer experience contact Caroline Pearson at CPearson@Avalere.com.
January 23, 11 AM ET
Learn More
