Fewer Highly Rated MA Plans in 2021 than in 2020
Summary
On October 8, the Centers for Medicare & Medicaid Services (CMS) published their 2021 Star Ratings for Medicare Advantage (MA-PDs) and standalone Prescription Drug Plans (PDPs) on Medicare Plan Finder.The Star Ratings program measures performance across several domains to provide beneficiaries information to support plan selection. Additionally, Star Ratings is linked to MA plan payment and quality incentives. MA plans with at least 4 stars can receive a higher benchmark and bonus payments that can be used to offer more benefits to beneficiaries at no extra cost. Each year, CMS updates the Star Ratings to incorporate clinical and stakeholder recommendations, new measures, and changes for measure improvement.
Highlights from This Year’s Star Ratings Report
Note: Avalere’s 2020 analysis measures the distribution of enrollees based on their 2021 Star Ratings. These enrollment percentages could shift in 2021 following the annual election period that runs until December 7.
Fewer MA-PD enrollees are in contracts with 4.5 stars. Approximately 19.6% of enrollees are in contracts with 4.5 stars, equating to an 11.8 percentage point decrease as compared to the share based on the 2020 Star Ratings. Furthermore, enrollment in 4-star-rated contracts is 7.9 percentage points lower, while enrollment in 3.5-star-rated contracts is 17.9 percentage points higher, going from 15.8% in 2020 to 33.7% in 2021.

Note: Avalere Health analysis and landscape assessment of 2021 MA-PD enrollment distribution is based on 2020 enrollment. Does not include plans without star ratings. Sources: “CMS Fact Sheet: 2021 Part C and D Star Ratings: 2019–2021,” October 8, 2018; October 9, 2019; and October 9, 2020.
More PDPs drop from 4 stars to a 3.5-star rating in 2021. The proportion of enrollees in PDPs with a 3.5-star rating in 2021 is 82% vs. 42% enrolled in PDPs with a 3.5-star rating in 2020, due to a reduction in the number of PDPs with 4 stars. Additionally, the enrollment distribution for PDPs with 3 stars is 1.8% in 2021 vs. 30.3% in 2020.
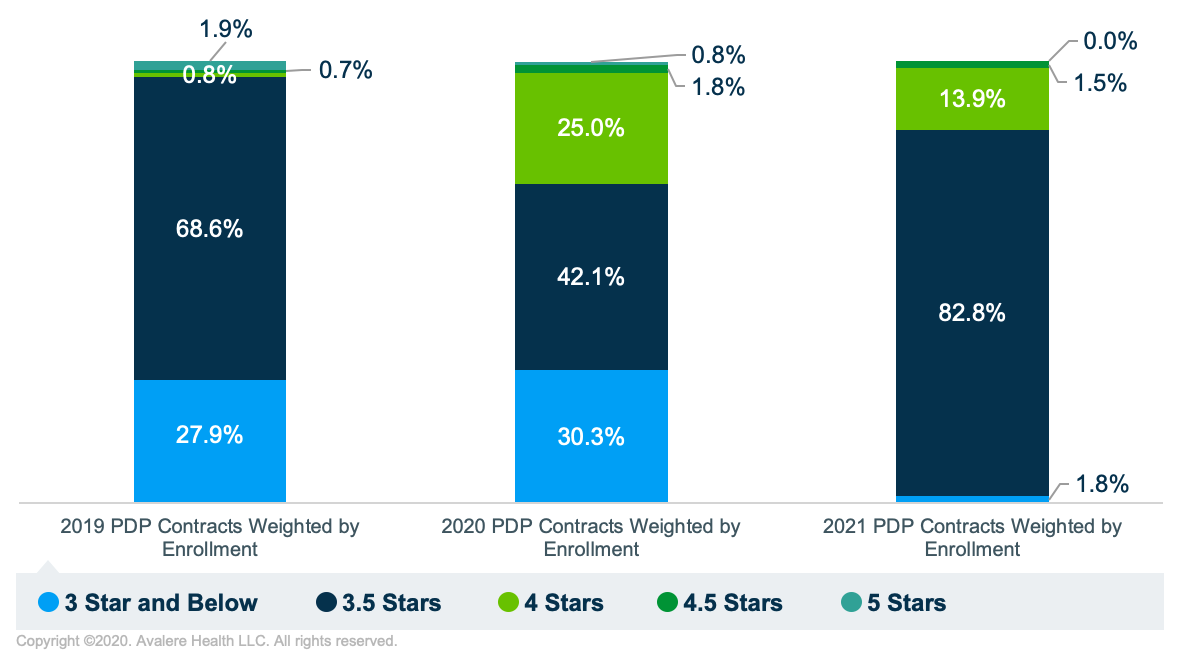
Note: Avalere Health analysis and landscape assessment of 2021 PDP enrollment distribution is based on 2020 enrollment. Does not include plans without star ratings. Sources: “CMS Fact Sheet: 2020 Part C and D Star Ratings,” October 9, 2019; “CMS Fact Sheet: 2021 Part C and Part D Ratings,” October 8, 2020.
Five million beneficiaries—nearly one-quarter of enrollees—are in MA-PDs that have a lower star rating in 2021 than in 2020. About 2.7 million beneficiaries are in contracts that dropped from a star rating of 4.5 stars in 2020. This reduction will have an impact on payment for 2022, as the star ratings for 2021 are used to determine payment for 2022.
| Measure Movement Category | Number of Contracts | Enrollment | Percent of MA-PD Enrollment |
|---|---|---|---|
| Gained 4 Stars | 19 | 289,331 | 2% |
| Gained 4.5 Stars | 20 | 813,931 | 4% |
| Gained 5 Stars | 8 | 191,716 | 1% |
| Dropped from 4 Stars | 31 | 1,327,099 | 7% |
| Dropped from 4.5 Stars | 24 | 2,758,943 | 15% |
| Dropped from 5 Stars | 5 | 453,142 | 2% |
| No Change | 244 | 12,497,593 | 68% |
Methodology
Avalere analyzed 2021 Star Ratings data released by the CMS. The analysis reflects contracts in the 50 states, DC, and the territories. Avalere excluded Employer Group Waiver, Program of All-inclusive Care for the Elderly, Cost, and Demo plans from the analysis. Avalere used plan and county-level enrollment from the October 2020 files.
For additional analysis and details on the CMS’s 2021 Star Ratings release and a look at how COVID-19 is reshaping quality improvement, we invite you to register for our upcoming webinar, “Achieving Star Ratings Excellence in a Brave New World,” presented by Inovalon® on November 5, 2020, 1–2 PM ET. The webinar will include data-driven strategies that you will need to support future operational and performance improvement initiatives. Register for this free webinar.
To learn more about how Avalere can help you, connect with us.







