SCOTUS Ruling on ACA Could Impact Coverage and Policy Outlook
Summary
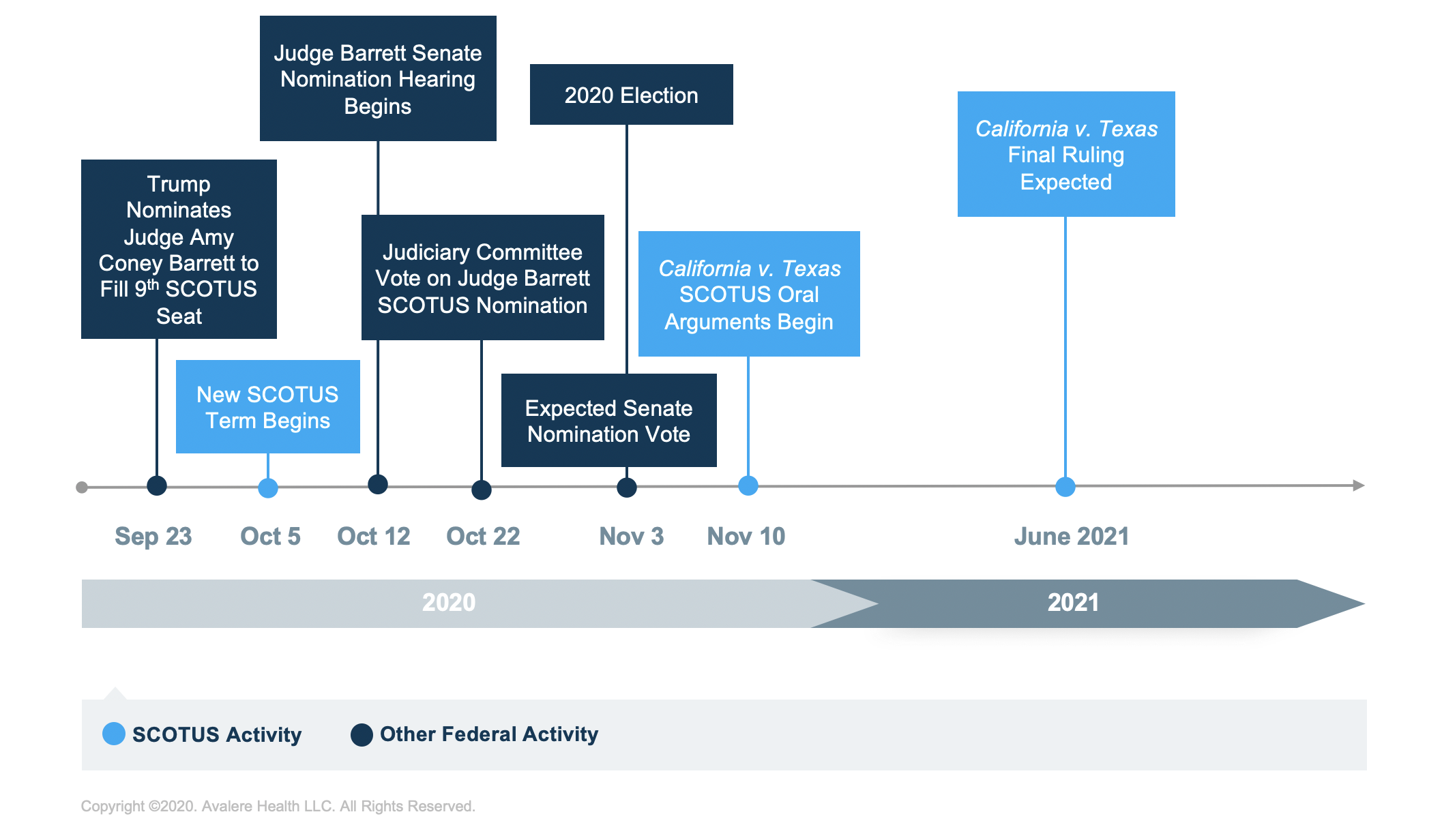
With the US Supreme Court set to hear arguments starting November 10 on California v. Texas, and Judge Amy Coney Barrett’s nomination under consideration in the Senate, questions remain regarding the future of the law.The California v. Texas litigation focuses on the constitutionality of the Affordable Care Act (ACA) following Congress’s decision to set the individual mandate penalty to $0 in the 2017 Tax Cuts and Jobs Act. In January, the US House of Representatives and Democratic attorneys general filed motion asking the US Supreme Court (SCOTUS) to review the 5th Circuit’s December 2019 ruling that the individual mandate is unconstitutional. Though the SCOTUS denied a motion to expedite the case during the court’s last term, it agreed to schedule oral arguments of California v. Texas on November 10. A final ruling is expected by June 2021.
Impact of New Justice Appointment on California v. Texas
Following the passing of Justice Ruth Bader Ginsburg, President Trump nominated Judge Amy Coney Barrett on September 26 to fill the vacant SCOTUS seat. As it is considered likely that Judge Barrett will be seated prior to November 10 and would be able to vote in the California v. Texas decision, a shift in the SCOTUS makeup introduces added uncertainty regarding the future of the ACA.
Potential Impacts
The SCOTUS’s review raises the issue of severability and, by extension, the constitutionality of the ACA’s coverage expansion and insurance market reforms. In addition to a ruling on the individual mandate, the SCOTUS could rule on whether other provisions of the law are severable from the mandate. If provisions or titles are deemed severable, the question of which could be struck down arises.
Following the passage of the ACA in 2010, the SCOTUS has reviewed multiple challenges to the law’s constitutionality, including the individual mandate, Medicaid expansion, contraceptive mandates, premium tax credits through Healthcare.gov, and the failure to pay risk corridor payments. In the case of partial or full invalidation, potential rulings vary in terms of likelihood and which coverage and access provisions would be impacted. Under partial invalidation, implementation may be settled in protracted litigation in the lower courts.

State Impacts
A variety of states have sought to enact statewide protections in their own laws that are specifically designed to guard against the possibility of the ACA being invalidated in the courts. Protections focus on pre-existing condition exclusions, coverage without cost-sharing for preventive services, and coverage for select or all essential health benefits (EHBs; e.g., prescription drug coverage, mental health and substance use disorder services). While some of the ACA’s market reforms apply to self-insured employer-sponsored plans, any changes to state law would only apply to individual and group insurance in the state. Under the ACA, EHB coverage requirements do not apply to self-insured employer-sponsored plans.
In 2019 and 2020, at least 18 states (CA, CT, DE, FL, HI, IN, LA, MD, ME, NH, NJ, NM, NV, NY, OR, VA, VT, and WA) enacted laws to establish protections against pre-existing condition exclusions or to stipulate coverage of all EHBs provided for in the ACA. By defining these coverage requirements in statute and removing explicit references to the ACA, states could maintain the authority to regulate coverage of EHB and other ACA provisions, even if invalidated by SCOTUS.
Irrespective of state approaches to these protections, however, a loss of federally funded subsidies (e.g., cost-sharing reductions, advance premium tax credits) and federal funding for reinsurance programs would significantly hinder states’ ability to support the same levels of coverage for beneficiaries.

Additionally, if the SCOTUS repeals Medicaid expansion provisions within the ACA, significant coverage disruption could occur in the 35 states and DC that have chosen to expand. The Medicaid expansion population may be forced to seek alternative forms of coverage or become uninsured.
Post-Election Outlook
While the Trump Administration has supported repealing the ACA, a September 24 executive order calls for protecting insurance coverage for individuals with pre-existing conditions. Vice President Biden has proposed additional exchange affordability provisions and reversing current Trump administration flexibilities for short-term plans and 1332 waivers.
Given that the oral arguments for California v. Texas shortly follow the November 3 presidential election, the SCOTUS ruling could have an impact on either administration’s health policy agenda in 2021 and beyond. In addition, should Democrats win the White House and Senate, the politics surrounding Judge Barrett’s nomination could make it more likely that Democrats would seek to eliminate the filibuster, shaping the potential health policy outlook regardless of the Court’s ruling.
To receive more expert insights on the latest healthcare news, connect with us.







