Medicare Part B Payment Increases Will Offset 340B Drug Reimbursement Cuts for 85% of Hospitals
Summary
Rural hospitals will see an average 2.7% net increase of Part B payments.New research from Avalere Health finds that 85% of hospitals will see a net increase in their overall Medicare Part B reimbursement as a result of recent Medicare outpatient payment changes.
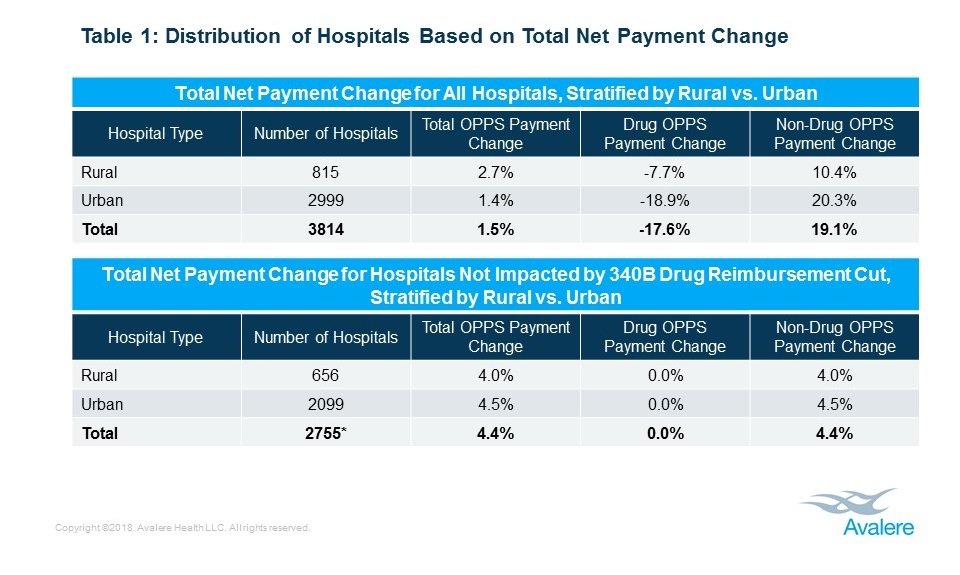
The changes, which took effect on January 1, 2018, cut reimbursement payments in the 340B drug program, which provides discounted outpatient drugs to health care facilities that serve low-income patient populations; however, the cuts will be offset by increases in other Medicare Part B payments (Table 1). Across all facilities, according to Avalere experts, hospitals will see an average 1.5% increase in their total Part B payments, and rural hospitals stand to benefit particularly, with those facilities netting a 2.7% increase in payments on average. Urban hospitals will see a 1.4% net increase (Table 2).
“Rural hospitals benefit the most from these payment changes, which effectively redistribute funds from urban hospitals and those participating in the 340B program,” said Joanna Young, senior director at Avalere.
Late last year, the Medicare Outpatient Prospective Payment System (OPPS) rule reduced Medicare’s payment to hospitals from average sales price (ASP) + 4.3% to ASP -23.7% for hospitals for Part B drugs purchased under the 340B program. This payment update will reduce Part B drug payments to the impacted hospitals by $1.6B in 2018. The savings of the 340B drug payment cut will be reallocated to increase reimbursements for other non-drug items and services paid under the OPPS.
Avalere’s analysis found that among the 15% of all hospitals that will experience a net payment reduction, the majority (76%) will see cuts less than 5% of their overall outpatient reimbursement. The research also found that more than half (55%) of total disproportionate share hospitals (DSH)—i.e., hospitals that serve a disproportionate number of low-income patients—will see payment increases more than offsetting the 340B drug reimbursement cuts.
“The Avalere analysis comes on the heels of a study published in The New England Journal of Medicine showing how hospitals have grown their 340B volume through acquisition of physician practices,” said Matt Brow, executive vice president at Avalere. “The Medicare payment changes reduce the financial benefit of 340B drugs to hospitals while increasing overall hospital payments and reducing beneficiary costs.”
On a state-by-state basis, the analysis finds that all but 8 states will experience a net increase in Part B payments as a result of this change (Figure 1).
Methodology
Avalere analyzed CMS’ hospital-level data on OPPS payments for CY2017 and CY2018 to determine the overall impact of the rule that captures both, 340B drug payment reduction and all other annual payment updates. CMS’s payment estimates reflect only rate updates and do not include changes in service volume, service-mix, or number of encounters, all of which would affect the actual payments to hospitals.
Avalere also analyzed 2016 Part B drug spending using the Medicare Standard Analytical File (SAF) that includes 100% of fee-for-service (FFS) drug billing by hospital outpatient departments (HOPDs). Avalere identified Part B drugs using the quarterly 2016 ASP Drug Pricing Files. Avalere excluded vaccines per OPPS rule. Avalere adjusted Part B drug payments for each hospital to simulate the payment under the new ASP -23.7% method and to assess impact of the reimbursement cut.
The analysis reflects 3814 hospitals paid under OPPS, not including 53 children’s and 11 free-standing cancer “held harmless” hospitals that receive proportional adjustments to their OPPS payment rates and are excluded from CMS’ impact file. Those hospitals are not subject to the Part B drug payment reduction even though they are 340B eligible. Similarly, Critical Access Hospitals and hospitals located in Maryland are eligible for 340B prices but are not paid under OPPS methods.
Avalere assessed current (as of January 2018) hospital 340B participation using the 340B Office of Pharmacy Affairs Information System (340B OPAIS) from Health Resources and Services Administration (HRSA)
The $1.6B Part B drug payment reduction estimate can be found at the CMS website.
Funding for this research was provided by the Community Oncology Alliance. Avalere maintained full editorial control.
To receive more expert insights on the latest healthcare news, connect with us.