Will Part D Redesign Lower OOP Costs for HIV Care?
Summary
The IRA’s Part D redesign could lower out-of-pocket costs for people with HIV; providers can help make sure their patients are aware of these changes.The Inflation Reduction Act (IRA) contains multiple drug-pricing provisions, including several reforms to the Medicare Part D benefit design. These provisions are expected to reduce out-of-pocket (OOP) costs for some beneficiaries, including people with HIV (PWH) who are enrolled in or will age into Medicare. Implementation of Part D redesign will reduce OOP costs for some Part D beneficiaries through the establishment of an OOP cap, the creation of an OOP smoothing program, and the expansion of the Low-Income Subsidy (LIS) program. As these provisions are implemented, HIV care providers can assist patients in navigating changes to the Part D benefit.
OOP Cap and Medicare Prescription Payment Plan
One of the primary policies in the IRA that is applicable to all Part D beneficiaries is the creation of an OOP cap at the catastrophic phase, beginning in 2024. In 2025, the catastrophic threshold and the OOP cap will be set at $2,000. This provision has the potential to reduce drug expenditures for PWH, as OOP costs for antiretrovirals often exceed $2,000 per year.
In addition to capping OOP spending, the IRA allows beneficiaries to smooth OOP costs over the course of a plan year through the Medicare Prescription Payment Program (MPPP). If a beneficiary opts into the MPPP, they can spread their cost sharing for a drug fill (up to the OOP cap of $2,000) across the remaining months in the plan year. The MPPP, in conjunction with the OOP cap, could reduce affordability challenges for those with high OOP costs early in the year, which may include PWH.
Providers can play an important role in educating their patients about these changing IRA Part D provisions. While Part D plans are required to notify all beneficiaries about the MPPP, additional patient outreach from HIV care providers and case managers could help ensure patients enrolled in Part D are aware of the program changes and how they will affect an individual’s monthly cost-sharing requirements.
LIS Expansion
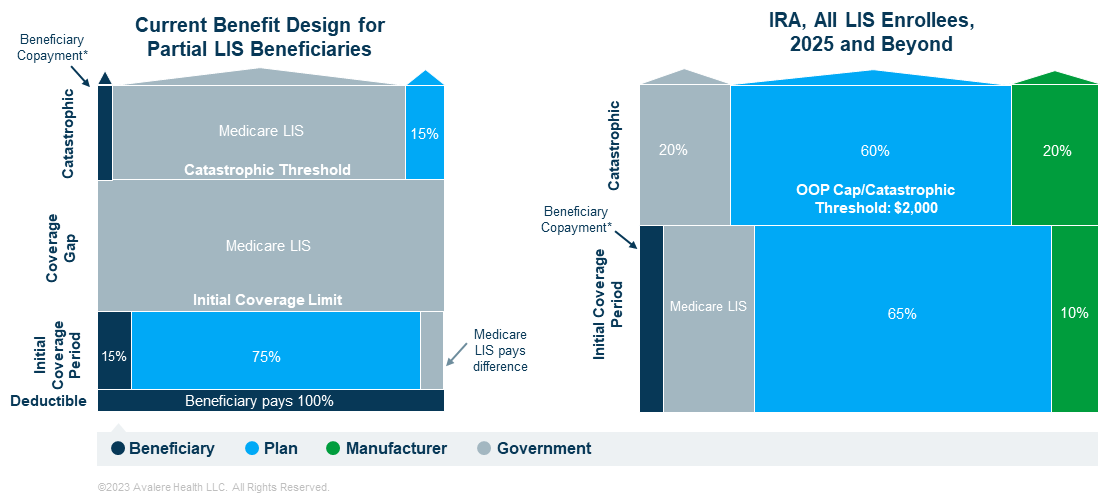
The IRA also contains affordability provisions aimed specifically at beneficiaries with low income through changes to the LIS program. The IRA rolls beneficiaries with the limited partial LIS benefit into the full LIS benefit. PWH who move from partial LIS to the full subsidy under the IRA will no longer pay a deductible and will have lower cost-sharing liability in the initial coverage period (Figure 1).
As with the OOP cap and MPPP, providers and case managers can help ensure that their patients are aware of these upcoming changes to the LIS program and how to enroll.
Dive Deeper
The IRA’s Part D redesign provisions aim to reduce affordability challenges and may significantly affect PWH. HIV stakeholders hope that addressing affordability challenges could increase access to antiretrovirals and potentially improve antiretroviral adherence.
As these policy changes are implemented, providers and Ryan White recipients can consider the impact on their practices, clinics, and the people they serve. The effects will likely vary across settings and over time as more PWH age into Medicare. As this shift occurs, providers can examine their payer mix and predict movement to Medicare over time. In addition, providers and patient groups can evaluate programs and services to identify ways to ensure PWH are aware of IRA programs to reduce OOP spending. Stakeholders should consider how to measure or model the impact of Part D redesign for PWH.
To learn more about how the IRA will impact PWH and HIV care providers, connect with us.







